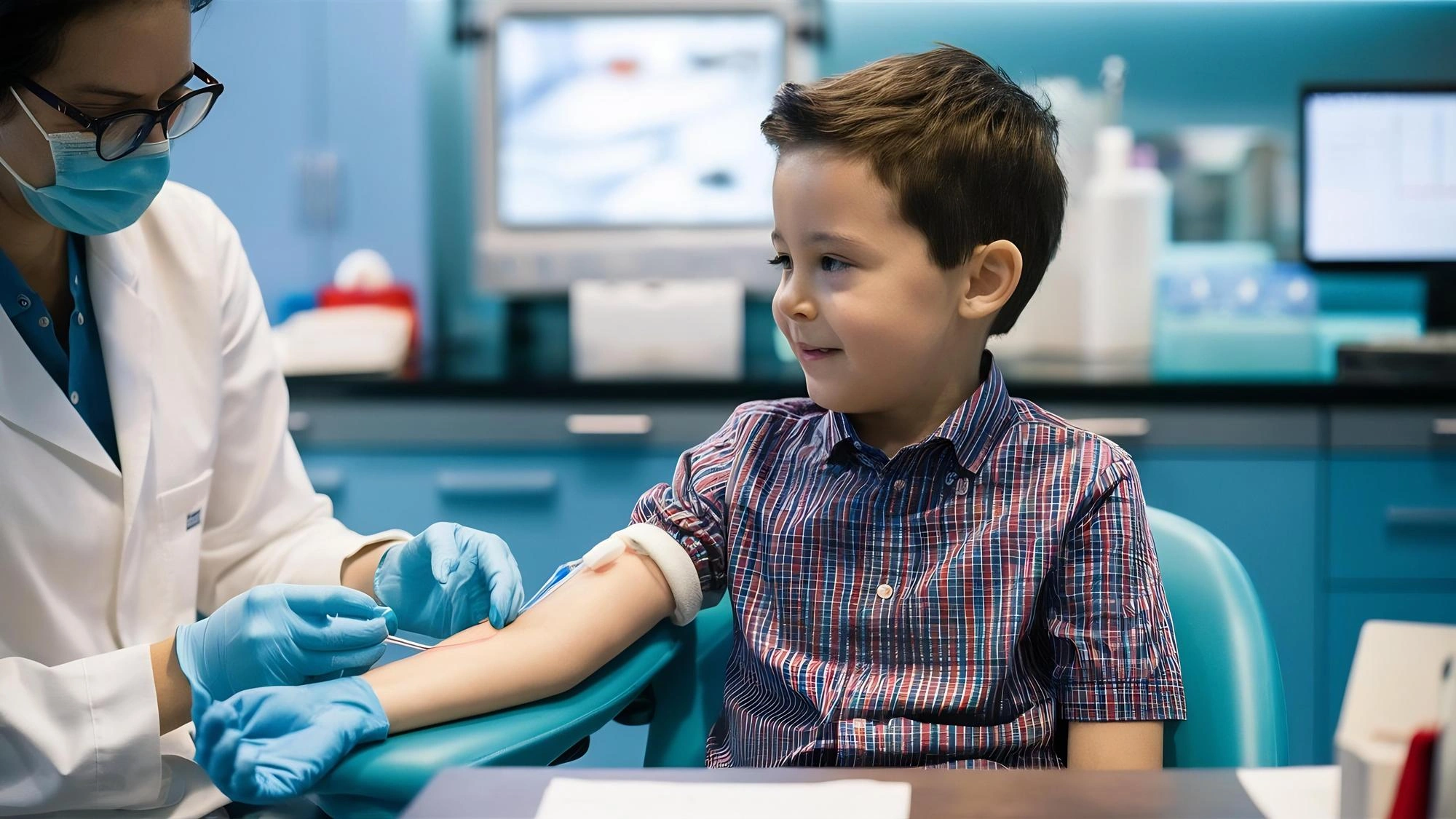
Expert Pediatric Hemato-Oncology Care in Chennai
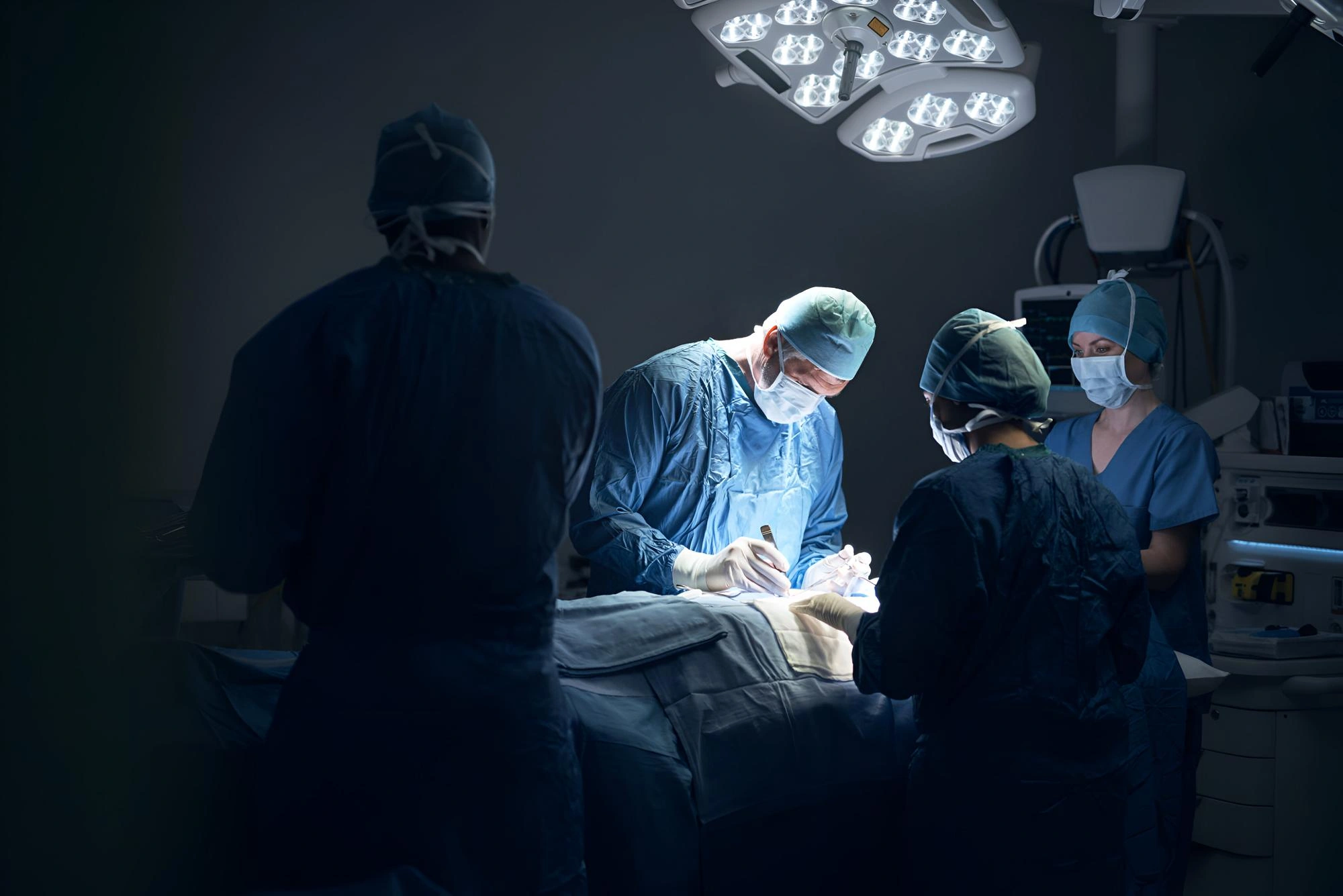
Pediatric Oncology is dedicated to the treatment of children with cancers. Our team of experienced pediatric oncologists is committed to providing comprehensive and compassionate care for young patients facing catastrophic diseases like cancer. We follow an organized, evidence-based practice setting to ensure each child receives the best possible treatment and support.

Types of Childhood Cancers We Treat
Hematological malignancies like Acute lymphoblastic leukemia; Acute myeloid leukemia; Chromic myeloid leukemia
Lymphomas like Non-Hodgkins lymphoma, Hodgkins lymphoma
Solid tumors like Neuroblastoma / wilms tumor / Germ cell tumors / Rhabdomyosarcomas
Bone tumors: Sarcomas: Ewings / Osteo
Brain tumors like medulloblastoma / low grade glioma / germ cell tumors / ependymoma
Langerhans cell histiocytosis
Dedicated Pediatric Oncology Ward for Chemotherapy & Care
There is a dedicated oncology ward for these children with dedicated 15 beds and two day care beds where maintenance of asepsis is given a priority for administering chemotherapy by a chemotherapy trained nursing staff. Treatment for each type of childhood cancer follows specifically designed protocols at our unit based on national and international guidelines.


Specialized Pediatric Cancer Treatments and Procedures
Depending on the type of cancer, treatment may include chemotherapy, surgery and / or radiotherapy. Majority of the chemotherapy is administered as inpatient with some being given as outpatient and day care chemotherapy. Children undergo procedures like Lumbar Puncture / Intrathecal drugs administration / Bone marrow aspiration & biopsy / accessing of implanted ports under appropriate procedural sedation. We have dedicated pediatric oncology nurses along with a pediatric oncology social worker who educate and support the entire family. Our social worker ensures a smooth experience for the child for the family throughout the treatment.
Why cancers in children are different from adults?
Cancer in children are different from that of adults. Children are not treated as miniature adults. They need a tailored approach to their cancers. They tolerate the chemotherapy better and have a better survival rates than adults. Taking a look at the survival rates of various cancers at our institute, we have had 80%-85% survival rate in the last 10 years.
Multidisciplinary team management:
Curing children with cancer requires a multidisciplinary effort. A team of doctors from various specialities (pediatricians / pathologists / radiologists / pediatric surgeons / nephrologist / neurologist / endocrinologists/ emergency physicians / intensivists) are available in house to provide their expertise in the treatment of children with cancer. A team discussion is done for every child with a difficult cancer and the best of available services are given to the ailing child. All such treatment offered is protocol and evidence based and we track all new healthcare research to provide the best to the child. The best of supportive care is given to these children for improving their outcomes. Not just during treatment but they are followed up through every stage of recovery.
Support for Underprivileged Children with Cancer – Ray of Light Foundation
Most of the children taking treatment at our hospital are from the lower socio economic strata and are under priviledged / lower middle class. We have Ray of Light Foundation to provide free treatment to children diagnosed with cancer-leukemias, to both lower and middle socioeconomic groups thereby contributing to the improvement of the outcome in these children. Additionally, hospital supports a few patients for their cancer treatment.




Pediatric Hematology
Pediatric Hematology is dedicated to providing comprehensive and compassionate care for infants, children, and adolescents with various hematologic conditions. With a team of experienced pediatric hematologists, nurses, social workers and support staff, we offer specialized services tailored to meet the unique needs of our young patients and their families.
Our services:
Bone Marrow Transplant:
The Ray of Light Foundation established the state-of-the-art Bone Marrow Transplantation (BMT) unit at our hospital. We started our first Bone Marrow Transplantation in year 2020.
The BMT unit, built in par with international standards, has dedicated air handling units (AHU) ensuring optimal patient safety. Additionally, 3 positive pressure rooms in the Intensive Care unit (ICU) for critically ill patients.
Transforming care:
This initiative aims to provide life-saving treatments for children facing cancerous conditions like relpased/refractory leukemia, lymphoma and non-cancerous conditions such as bone marrow failure, immunodeficiency, and hemoglobinopathies like thalassemia & sickle cell anemia and metabolic disorders.
From matched family and unrelated donors to innovative techniques like Haploidentical PTCY and Haploidentical TCR alpha/beta depleted HSCT, we are expanding treatment options for every child.
Our dedicated multidisciplinary team involving pediatric hemato-oncologists, transplant specialists, transfusion medicine experts, intensive care professionals, infectious disease specialists, pediatric surgeons, neurosurgeons, neurologist, endocrinologist, anaesthetist, competent nurses and social workers is unwavering in its commitment to providing ongoing care, support, and expertise to ensure the long-term well-being of post BMT children.





Speciality Clinics:
We offer dedicated speciality clinics for children with a diverse range of blood disorders. Our specialized clinics are designed to provide comprehensive care and support for patients and their families, ensuring the highest quality of evidence based treatment and management for each condition.
Pediatric Blood disorders:
We specialize in diagnosing and managing a broad spectrum of pediatric blood disorders, including various causes of anemia, thrombocytopenia, bleeding disorders, thalassemia, sickle cell disease, bone marrow failure and immunodeficiency. Based on evidence-based guidelines and multidisciplinary discussions, especially in challenging cases, we ensure the highest standard of care for our patients.
Genetic Counselling:
With the assistance of genetic specialists, we offer comprehensive genetic counselling to families at risk of inherited blood disorders. Our aim is to provide information, support, and guidance, empowering families to make informed decisions about their child’s health and future.
Psychosocial Support:
Our social workers and support staff offer emotional support, counselling, and resources to assist families in coping with the challenges of managing chronic blood disorders.
After treatment follow-up clinic:
Treatment for children with cancer doesn’t end with completion of the designated treatment, but they need follow up beyond their treatment period. All our cancer children who have completed treatment are seen in the follow up clinic and the necessary rehabilitative services are given. This also ensures that they return to the school life without any stigma.
Thalassemia clinic:
Our Thalassemia Clinic offers comprehensive care, encompassing blood transfusions, iron chelation therapy, supportive care, genetic counselling and the curative bone marrow transplantation.
Bleeding disorders clinic:
We specialized in diagnosis and management of Haemophilia, Von Willebrand disease, platelet dysfunction and other rare bleeding disorders. We provide comprehensive treatment plans including factor replacement therapy, joint protection and emergency management of bleeding episodes.
Primary immunodeficiency clinic:
Primary immunodeficiency disorders are genetic defects of immune system can lead to life threatening infections and autoimmune manifestations. Early diagnosis and timely intervention including bone marrow transplantation, when necessary, can profoundly transform their lives. We perform thorough evaluations, including advanced diagnostic testing and genetic screening when necessary to ensure accurate diagnosis. We provide comprehensive care, including appropriate management of infections with the assistance of infectious disease specialists, immunoglobulin replacement therapy, education to minimize infection risk, and ongoing monitoring.We have performed successful transplants for children with these disorders.
Meet the Leading Pediatric Hemato-Oncologists
KKCTH pediatric hemato‑oncologists are highly experienced in treating children with cancers and blood disorders. Their expertise spans leukemia, lymphomas, solid tumors, and rare hematologic conditions. Every child receives a personalised plan grounded in evidence and a precise diagnosis. The team works closely with pediatric surgeons, intensivists, and other specialists to deliver coordinated care. Families receive counselling that combines medical excellence with emotional comfort.
FAQ
- KKCTH's Paediatric Haemato-Oncology department, led by Dr. Arathi Srinivasan (Senior Consultant and Head, Post-Doctoral Fellowship Haemato-Oncology) and Dr. S. Meena (FNB Paediatric Haemato-Oncology), treats the full spectrum of childhood malignancies.
- Cancers managed include haematological malignancies (acute lymphoblastic leukaemia, acute myeloid leukaemia, chronic myeloid leukaemia), lymphomas (Hodgkin and non-Hodgkin), and solid tumours (neuroblastoma, Wilms tumour, rhabdomyosarcoma, germ cell tumours). Bone tumours (Ewing's sarcoma, osteosarcoma) and brain tumours (medulloblastoma, low-grade glioma, ependymoma, germ cell tumours) and Langerhans cell histiocytosis are also managed. The department has achieved an 80–85% survival rate across all childhood cancers over the past 10 years.
- Yes. The department provides comprehensive management of paediatric haematological disorders including thalassaemia, haemophilia, sickle cell disease, aplastic anaemia, and primary immunodeficiency.
- Speciality clinics operate for thalassaemia (blood transfusions, iron chelation, BMT evaluation), bleeding disorders (haemophilia, Von Willebrand disease—factor replacement therapy, joint protection), and primary immunodeficiency (diagnostic evaluation, immunoglobulin replacement, infection prophylaxis). Genetic counselling with the medical genetics team is available for families at risk of heritable blood disorders. Bone marrow transplantation—commenced in 2020 through the Ray of Light Foundation is available for children with relapsed leukaemia, lymphoma, aplastic anaemia, thalassaemia, and immunodeficiency.
- Yes. Chemotherapy is administered in a dedicated 15-bed oncology ward and a day-care facility, staffed by chemotherapy-trained nursing personnel under strict aseptic conditions.
- Treatment protocols are based on national (ICMR) and international (COG, SIOPE) evidence-based guidelines, with adaptation for patient-specific factors. Chemotherapy is delivered as inpatient, outpatient, or day-care depending on the regimen intensity and patient stability. Procedural sedation is available for lumbar punctures, intrathecal chemotherapy, bone marrow aspirates, and port access. Dr. Arathi Srinivasan's team conducts multidisciplinary tumour board discussions for every complex case.
- Yes. Infection prevention is a primary concern in paediatric oncology, as chemotherapy-induced immunosuppression places children at high risk of life-threatening sepsis.
- The dedicated oncology ward maintains strict aseptic protocols, hand hygiene standards, and visitor restrictions. Three positive-pressure isolation rooms in the BMT unit's ICU provide additional protection for post-transplant patients. Infectious disease specialists are available in-house to guide empirical and targeted antibiotic therapy during febrile neutropenia episodes. Prophylactic antifungal and antiviral agents are employed as per protocol, and the immunisation status of all oncology patients is reviewed at diagnosis.
- Yes. A paediatric oncology social worker provides psychosocial support, counselling, and practical assistance to patients and families throughout the treatment journey.
- The social worker helps families navigate financial concerns (the Ray of Light Foundation provides free treatment to eligible leukaemia patients from lower and middle socioeconomic backgrounds), school reintegration, and emotional adjustment to diagnosis and treatment. Families receive education regarding treatment protocols, side effect management, and the importance of treatment adherence. Post-treatment follow-up clinics also address survivors' educational reintegration, aiming to ensure children return to school life without stigma.
- Yes. Cancer treatment in children does not end with completion of the designated protocol long-term surveillance for late effects, recurrence, and rehabilitation is an essential component of care.
- Late effects of chemotherapy and radiotherapy include cardiomyopathy, endocrine dysfunction, neurocognitive impairment, secondary malignancies, and growth disturbance. KKCTH's dedicated follow-up clinic for completed-treatment oncology patients monitors these outcomes systematically, with input from cardiology, endocrinology, neurology, and rehabilitation services as required. This commitment to survivorship care recognises that children cured of cancer deserve optimal long-term quality of life.